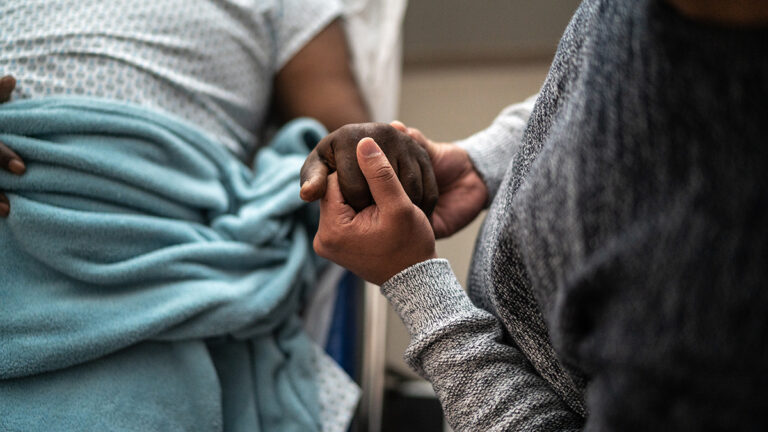
The four months of care Annie Mae Bullock received for her stage 4 lung cancer were rocky at best. But the final three days of that care, her daughter Karen Bullock said, were excellent.
Annie Mae spent those few days in hospice care at home surrounded by loved ones singing, chanting and praying as she passed.
Listen to this story here.
“We did all of the things we knew she would have wanted us to do,” Karen Bullock said. “And we didn’t have to worry about whether we were being judged.”
That was one of the few times during those hard four months that Bullock and her family hadn’t felt judged. They felt judged when Annie Mae initially declined chemotherapy and later on, when she asked why she needed a legal document outlining her end-of-life wishes.
Bullock is grateful that her mother had those days at home in hospice. She knows many Black families don’t get them.
Research shows that, for seriously ill patients, high-quality supports like advance care planning, hospice and palliative care can alleviate suffering for them – and their families. Benefits include reduced pain and emotional distress, and fewer unwanted interventions.
But Black patients, who are at greater risk for many serious illnesses, are less likely to receive these supports than White patients. For example, just 35 percent of Black seniors eligible for hospice care through Medicare actually receive it, compared to 50 percent of White Medicare beneficiaries.
A lonely road
This is a world Bullock has personal and professional experience navigating. She is a licensed clinical social worker and professor at the Boston College School of Social Work. And for the last two decades, Bullock has been studying why seriously ill Black patients – with incurable conditions like cancer or kidney failure – are less likely to get palliative care, and what it would take to change that.
“In retrospect, seeing that my mother could actually die well is what set me on this journey,” Bullock said.
She has struggled to find funding for her work, told repeatedly to focus on other topics or use data sets that already exist.
“But the large data sets don’t answer the questions that have not yet been asked,” Bullock said.
Through two decades of persistence amassing small studies and focus groups, and the work of others, Bullock has identified some of the barriers. The two biggest, she said, are the failure of the U.S. health care system to build trust with Black families and a lack of culturally competent care.
A system that can’t be trusted in life or in death
America’s legacy of racism runs deep throughout its health care system, shaping the care Black patients receive and the medical decisions they make – including at the end of life, according to Bullock.
She recalled conversations with Black seniors who remember when their local hospital was segregated or when their communities were targeted with toxic waste sites.
“It’s difficult to convince someone that there is a team of people who want you to die well, when nobody cared if you lived well,” Bullock said.
Racial bias still exists in health care today. Nearly 1 in 3 Black adults in a recent survey said they had been treated poorly by a health care provider because of their race or ethnicity. More than 20 studies document that seriously ill Black patients are less likely to have their pain properly treated, diagnosed or managed.
Bullock said it is a rational decision for people to reject services from a system that has not proven trustworthy.
A culturally incongruent model of care
Bullock has focused a lot of her work on hospice – the kind of end-of-life care that benefitted her own mom. It often happens at home and is free of aggressive intervention.
But after studying the care experiences of more than 1,000 older Black adults and caregivers, Bullock came to the conclusion that certain aspects of the hospice care philosophy, which originated in Europe, are what she calls culturally incongruent.
“This is a European model of care that many White people find to be extremely helpful in dying a good death and having their needs met until the end,” Bullock said.
But she points to the spiritual care component of hospice as one common source of incompatibility. Surveys show spirituality plays a much larger role in the lives of Black families, but White hospice workers may not be familiar with those religious traditions and beliefs.
The least ideal time to explain your cultural preferences, said Bullock, is when you are sick or dying.
“When a patient and or family member has to educate you about their culture while they are receiving care, the message you’re sending is, ‘I don’t know anything about you. I haven’t learned to take care of you,’” she said.
A path toward more equitable care for the seriously ill
For years, experts have been calling for greater equity in care for the seriously ill and dying, but the COVID-19 pandemic has brought renewed attention to the issue.
Some experts, including Bullock, are prioritizing collecting better data and diversifying the medical workforce. Others are focused on expanding access to palliative care, which offers much of the same physical, emotional and spiritual support as hospice without requiring patients to cease aggressive interventions. Research shows Black patients tend to prefer having more intensive treatment options available even at the end of life.
Additional attempts to reduce racial disparities include programs that engage Black churches to reach more patients and those that offer more culturally tailored palliative care. More research is needed to evaluate the effectiveness and scalability of these and other interventions.
Bullock acknowledged working on health care equity can sometimes feel like shouting into a void. On especially hard days she returns to the memory of her mother’s final moments.
As Annie Mae appeared to lose consciousness, Bullock’s family wondered if they should continue their praying and singing and chanting.
It was the hospice social worker who explained the hospice philosophy that hearing is the last sense to go, and gave them a piece of advice Bullock will never forget.
“Continue to say the things you want to say,” the worker urged the Bullock family. “She can hear you even if she can’t respond.”
This story comes from the health policy podcast Tradeoffs, a partner of Side Effects Public Media. Dan Gorenstein is Tradeoffs’ executive editor, and Leslie Walker is a senior producer for the show, which ran this story on Nov. 10, 2022. This Tradeoffs story is part of a series on complex care supported by the Better Care Playbook.