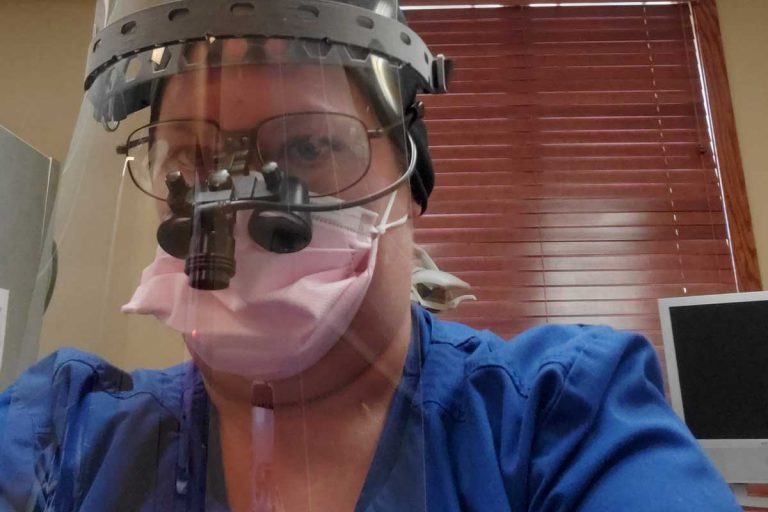
Even without a global pandemic, dentistry is inherently riskier than many other medical professions.
That’s because dentists and hygienists spend a lot of time inches away from wide-open mouths, conducting procedures known to generate aerosols — tiny droplets that can linger in the air and carry viruses.
So when dental hygienist Jeanne Bosecker started back at work in mid-May, she says it felt a little soon to be reopening for routine dental care.
But once she learned about the infection control precautions her office in the northwest Chicago suburbs was taking, she felt more comfortable.
The large office space allows Bosecker and co-workers to spread out, which she feels minimizes the COVID-19 risks to her and her patients. She is also taking steps to reduce aerosols — scraping teeth by hand, instead of using the ultrasonic machines that spray air and water.
Her office initially did not have N95 masks, which are recommended by the Centers for Disease Control and Prevention to prevent infection from patient aerosols.
In that case, CDC guidance says a surgical mask and a face shield can be used instead.
Bosecker felt protected with that. But not all hygienists do, especially if they or members of their household are at higher risk of getting complications from COVID-19.
“I have a friend who has asthma, and her dentist isn’t providing the N95 mask,” Bosecker says. “And she doesn’t want to return to work without that as a minimum.”
At the start of the COVID-19 pandemic, dental offices across the nation canceled routine visits and began limiting visits to emergency care. In recent weeks, nearly all states have allowed dentists to completely reopen.
Guidelines from both federal and state agencies urge dentists to take numerous precautions to protect staff and patients from COVID-19. These include wearing masks and gowns at all times, screening everyone for COVID-19 symptoms, installing air filtration systems and using techniques that reduce aerosol generation.
But even with efforts to minimize the risks, some who work in dentist offices are left wondering if reopening is the right move.
Dentists struggle to acquire personal protective equipment
Part of the problem is that at the start of the COVID-19 pandemic, dentists were asked to donate their PPE to the frontlines, says Bosecker, who serves as president of the Illinois Dental Hygienists Association.
“And now they’re having trouble getting it back,” she says.
Hygienists have shared concerning stories onto her organization’s Facebook page about dentists asking staff to work without providing adequate protective gear, Bosecker says.
Some say they’re being asked to not change masks and gowns between patients, in violation of state and federal guidelines.
Bosecker says she recently brought these issues to the leaders of the Illinois dental society.
“And they kind of acted like, ‘Oh, well, you know, none of our members would ask our staff to work without the appropriate PPE,’” she says. “They’re in denial that it’s happening.”
Bloomington-based dentist Stacey Van Scoyoc, who serves as vice president of the Illinois State Dental Society, says they’re not in denial about the possibility that some dentists want to reopen without the appropriate protective equipment on hand.

But the dentists she knows who are struggling to get the right gear are waiting to reopen, she says.
Van Scoyoc says dentists have completely changed the way they operate to minimize risks.
Offices are screening patients for COVID-19 symptoms prior to their visit and on the day of, she says.
Many are spacing out appointments, not allowing visitors unless absolutely necessary, and taking other precautions, such as offering early morning time slots to those in high-risk categories to minimize their exposure to prior patients’ aerosols.
Van Scoyoc says the dental society is instructing members to contact legislators to get dentists ranked higher on the state emergency management agency’s PPE priority list, which would help ease the challenges many dentists are facing with PPE shortages.
“Hopefully soon, the supply will match the demand for all of us in the healthcare professions,” she says.
Uncertainties create additional challenges
Many who are concerned about the risk of exposure to COVID-19 in dentist offices cite a commonly referenced study from the New England Journal of Medicine that finds coronaviruses in aerosols can linger in the air for three hours.
But since that study was conducted in a highly controlled lab environment, it’s not clear the findings extend to aerosols created in dentist offices, says Purnima Kumar, a periodontist and microbial ecologist at Ohio State University’s college of dentistry.
Dental aerosols are often diluted with water, which would lower the amount of virus present in particles, Kumar says.
And there’s currently no evidence that the novel coronavirus is showing up in dental aerosols from patients who are not showing COVID-19 symptoms. (The CDC recommends screening patients for symptoms prior to their visits).

“But that evidence is not available because nobody has looked for it,” Kumar says. “So, absence of evidence is not evidence of absence.”
In other words, the risks can’t be ruled out. Even the CDC has said it’s too early to know for sure whether standard precautions adequately protect dental workers from exposure to COVID-19.
Following the guidelines is not a requirement for licensure, Van Scoyoc says, and how the guidelines are implemented will look different in every office.
Kumar says there’s no “one-size-fits-all” solution, given the myriad differences between dental practices.
Instead, dentists must use their professional judgment in determining how to minimize risks to the greatest extent possible.
But how much caution is enough?
The challenge comes when employees disagree with supervisors about what level of precaution is appropriate and necessary.
Alex, a dental hygienist in the north Chicago suburbs, says she’s back at work but doesn’t think her office has enough air filtration units for the size of the space. Illinois Newsroom is using only her middle name because she worries speaking out could cost her her job.
“I was told that I need to leave my fears at the door and carry on and act as if everything is fine,” Alex says.
She says a lot of hygienists don’t feel safe going back, but have no choice because they’ve been out of work and have bills to pay.
She says employees can express their concerns, but dentists and practice owners ultimately have the final say.
Sara Mercier, a dental hygienist and former president of the Nevada’s hygienists association, says she operates a Facebook group about ethics for hygienists.
She has heard from hygienists across the country who are concerned about the risks of reopening for routine dental care.
“This is a really big concern for us as far as our ethics to ‘do no harm,’” Mercier says. “We can’t guarantee right now that we’re doing no harm to patients.”
The CDC urges dentists to “prioritize the most critical dental services,” to minimize the harm to patients who could develop worse problems if they delay care — and to workers from potential exposure to COVID-19.
Van Scoyoc says her office is taking that approach.
She says her advice to patients wondering whether to come in for non-emergency care will depend on several factors:
How serious are their dental health needs? What are their individual COVID-19 risk factors? And how comfortable do they feel coming into the office?
She says dentists, and all health care providers, want to help patients feel safe so that no one puts off needed care.
This story was produced by Side Effects Public Media, a news collaborative covering public health. Christine Herman is a reporter at Illinois Public Media. Follow her on Twitter: @CTHerman