URBANA – Three large hospital systems in central Illinois — Carle Health, Memorial Health System and OSF HealthCare — are seeing more COVID-19 patients than ever before.
Carle and Memorial — which each operate five hospitals across central Illinois — recently released public dashboards showing both the number of hospitalized patients and the percentage of positive COVID-19 tests has been trending upward since late summer.
The hospital metrics signal the virus is taking off in the region like never before. Carle spokeswoman Jamie Mullin says there are serious ripple effects if hospital beds fill up.
“It’s not just about COVID anymore,” she says. “It’s about: How do we, as the region’s Level 1 Trauma Center, make sure we have space to care for the things that are still going to happen everyday,” such as car accidents, heart attacks, strokes and other medical emergencies that don’t pause during a global pandemic.
The best thing people can do to help hospitals not get overwhelmed is heed public health guidance aimed at stopping the spread of the virus.
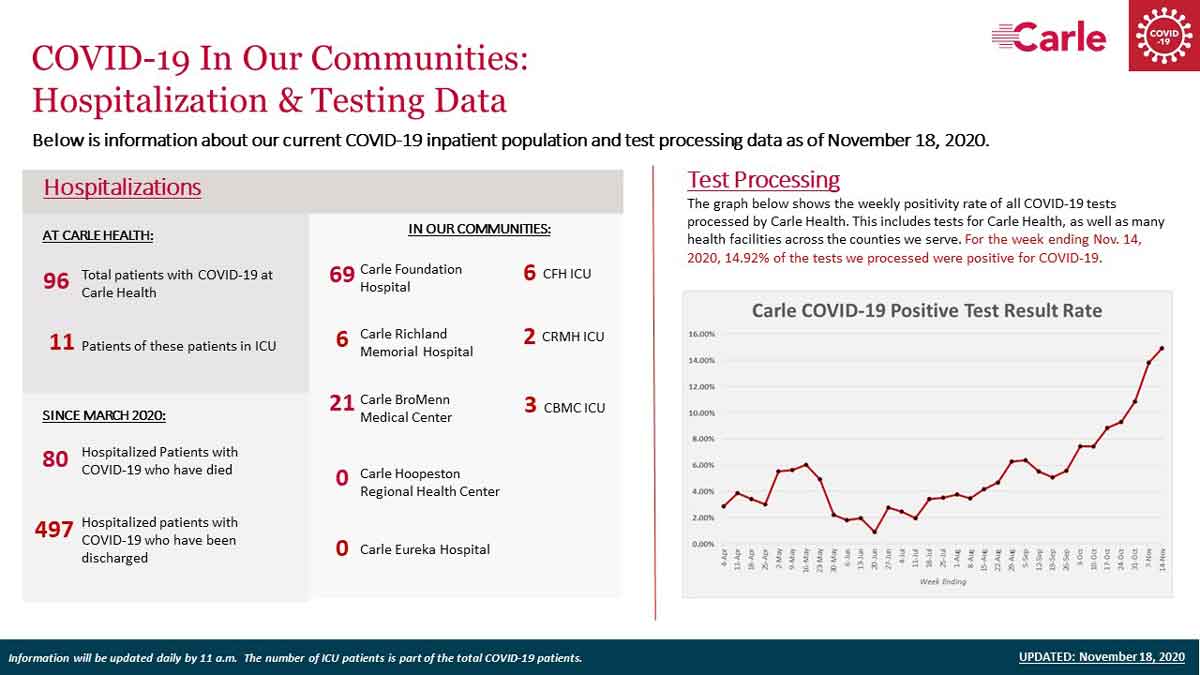
Since March, 673 people have been hospitalized with COVID-19 at Carle. Currently, 96 are hospitalized, 497 have been discharged and 80 have died.
As of Wednesday, 69 patients are hospitalized with COVID-19 at Carle Foundation Hospital in Urbana — with 6 patients in the ICU. Six patients at Carle Richland Memorial in Olney and 21 patients at Carle BroMenn Medical Center in Normal are also receiving treatment for the virus — with five total ICU patients at those facilities. (There are currently no COVID-19 patients at Carle’s Hoopeston and Eureka locations.)
In an effort to ensure hospital beds are available for the sickest patients, Carle launched a program, “COVID @ Home,” in September, to provide virtual monitoring for COVID-19 patients from home.
So far, 82 patients who sought care at the emergency department in Urbana were deemed eligible for the program and enrolled — and most of them were able to recover safely at home. Only about 15% ended up needing to be hospitalized, says Lynne Barnes, Carle Foundation Hospital president.
Patients are provided with a thermometer and device to measure oxygen levels in their blood — in addition to instructions for self-care. Providers check in with them once or twice a day, and patients are able to reach out to the hospital for virtual care as needed.
“The same provider is talking to the patient each day,” Barnes says. “That way, you know what their voice sounds like, you know how they’re kind of coming along, you’re able to compare better. We’ve found that that’s been a good trick of the trade.”
Barnes says Carle has plans in place to expand capacity as needed.
But hospital leaders are also asking everyone to do their part to prevent the spread of the virus.
Back in the spring, Barnes says Carle was prepared to respond to a surge in cases, but thanks to the stay-at-home order and other COVID-19 mitigations, the number of cases were much lower than expected.
“That was extremely fortunate, we kind of saw that flattening of the curve,” says Barnes, who estimates Carle was caring for no more than a dozen patients at any point early on in the pandemic.
Throughout the summer, numbers ticked up slowly. Then in October, Barnes says cases started to take off.
“During the week of Oct. 4… we had a positivity rate of about 7.45%, out of nearly 6,500 tests,” Barnes says. “This past week [the week of Nov. 8], we did over 10,000 tests, and have a positivity rate of 14.92%.
The overall number of COVID-19 patients testing positive at Carle has also increased, she says: 1,500 cases last week, compared to less than a third that many the week of Oct. 4. (Memorial Health System — which operates hospitals in Springfield, Decatur, Taylorville, Lincoln and Jacksonville — has been seeing a similar upward trend.)
In addition to the “COVID @ Home” program aimed at providing care outside of the hospital whenever possible, Barnes says Carle has plans in place to increase staffing, equipment and hospital beds in the event that the region’s needs grow beyond the current capacity.
“We’ll be able to expand and manage what’s coming through the door,” Barnes says.
OSF HealthCare — which operates hospitals in Urbana, Danville, Peoria and Bloomington — offers a similar virtual care program for patients, known as “Acute COVID @ Home.” Spokeswoman Libby Allison said more than 1,400 patients have participated as of Tuesday.
Asked for specifics regarding COVID-19 hospitalization and test positivity rates, Allison said via email that OSF is seeing a “steady increase in the number of COVID-19 patients across all of our hospitals.”
She said OSF provides data regarding patient numbers, ICU and hospital bed capacity to local health departments daily, but is not publicly reporting the numbers as other hospital systems are.
“We look to the health departments in every community we serve to be the single source of truth for hospitalized COVID patients and bed capacity in that county,” Allison said. “This is to help reduce potential duplication or redundancy in the count.”
The rise in community transmission of the coronavirus has prompted “Tier 3” mitigations at the state level, aimed at preventing Illinois’ hospitals from becoming overwhelmed.
Beginning on Fri, Nov. 20, additional restrictions on certain businesses — including casinos, museums, movie theaters and banquet halls — will take effect. The restrictions fall short of a stay-at-home order, but Gov. J.B. Pritzker is urging residents to refrain from gathering with people outside of one’s household and limit nonessential activities as much as possible.
The Illinois Hospital Association issued a statement saying it supports Pritzker’s decision to help mitigate the “alarming surge” in COVID-19 infections and hospitalization.
“Hospitals in every area of the state now have higher caseloads of COVID-19 patients than they faced during the spring surge,” said IHA President A.J. Wilhelmi. “We urge everyone to follow these simple but very effective public health measures: wear a mask, watch your distance, wash your hands, avoid large family and social gatherings, and get a flu shot.
“All of us must act now and work together to protect our families, friends, neighbors, and the healthcare workers who are selflessly serving our communities.”
If you have a question you would like Illinois Newsroom to address regarding COVID-19, submit it here.
Christine Herman is a reporter with Illinois Newsroom. Follow her on Twitter:@CTHerman

